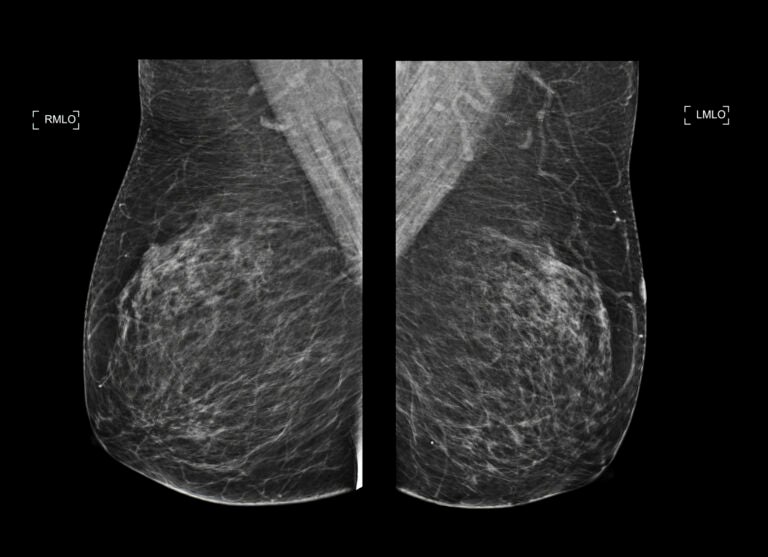
In a significant development, healthcare providers in Pennsylvania are now utilizing mammograms to detect early signs of heart disease in women. Traditionally used for breast cancer screening starting at age 40, these imaging tests are revealing important information about cardiovascular health by examining calcium buildup in the blood vessels of the breasts.
This calcium buildup, which appears as bright white lines or clusters on X-ray images, was previously thought to have no connection to heart disease. However, recent research indicates otherwise. According to Dr. Matthew Nudy, a noninvasive cardiologist and assistant professor at Penn State College of Medicine, the presence of these calcium deposits, known as breast arterial calcification (BAC), signals a higher risk of heart attack, stroke, or other cardiovascular complications as women age.
Linking Mammograms to Heart Health
Many women over the age of 40 have undergone mammograms, which makes them a practical tool for assessing heart disease risk. As Dr. Nudy explains, while coronary artery calcium scans are typically used to assess cardiovascular risk, mammograms can provide similar insights with a larger patient population. “It’s already being done for breast cancer screening across large numbers of patients in the population,” he noted.
Since August 2023, Jefferson Health hospitals in the Greater Philadelphia area have begun incorporating BAC information into their mammogram screening reports. Patients receive educational flyers prior to their screenings, detailing what BAC is and how it may impact their cardiovascular health. This initiative aims to empower women with knowledge that could lead to improved heart health.
Understanding the Implications of BAC
The detection of BAC is not merely an academic exercise; it has practical implications for women’s health. Dr. Jason Shames, assistant professor of radiology at Thomas Jefferson University, emphasizes the importance of this information in encouraging proactive health measures. “If a patient knows that they have a BAC, they may be more in tune with what their blood pressure is, more likely to get medications, and more aware of their health,” he stated.
Radiologists now review each mammogram for signs of BAC and include this information in the reports sent to patients. This enables physicians to guide women toward specialists for further cardiovascular evaluations if necessary. Additionally, Jefferson Health, in collaboration with Solis Mammography, offers a program called Mammo+Heart. This service utilizes artificial intelligence to analyze BAC more comprehensively, although it comes at an additional cost for patients opting in.
While the absence of BAC does not eliminate heart disease risk, discovering it through mammograms provides an opportunity for early intervention. Experts recommend that women discuss these findings with their primary care providers and consider lifestyle changes or medications to mitigate their risk.
As Dr. Nudy points out, further research is needed to understand the impact of BAC notifications on patient behavior and health outcomes. “Does that maybe increase statin uptake? Does that mean patients lead a healthier lifestyle? Does it actually lead to fewer heart attacks, strokes, and deaths over time?” he asked, highlighting the potential for BAC detection to alter the course of women’s health.
This innovative approach to using mammograms for heart disease risk assessment represents a promising intersection of breast and cardiovascular health, paving the way for more comprehensive healthcare for women.