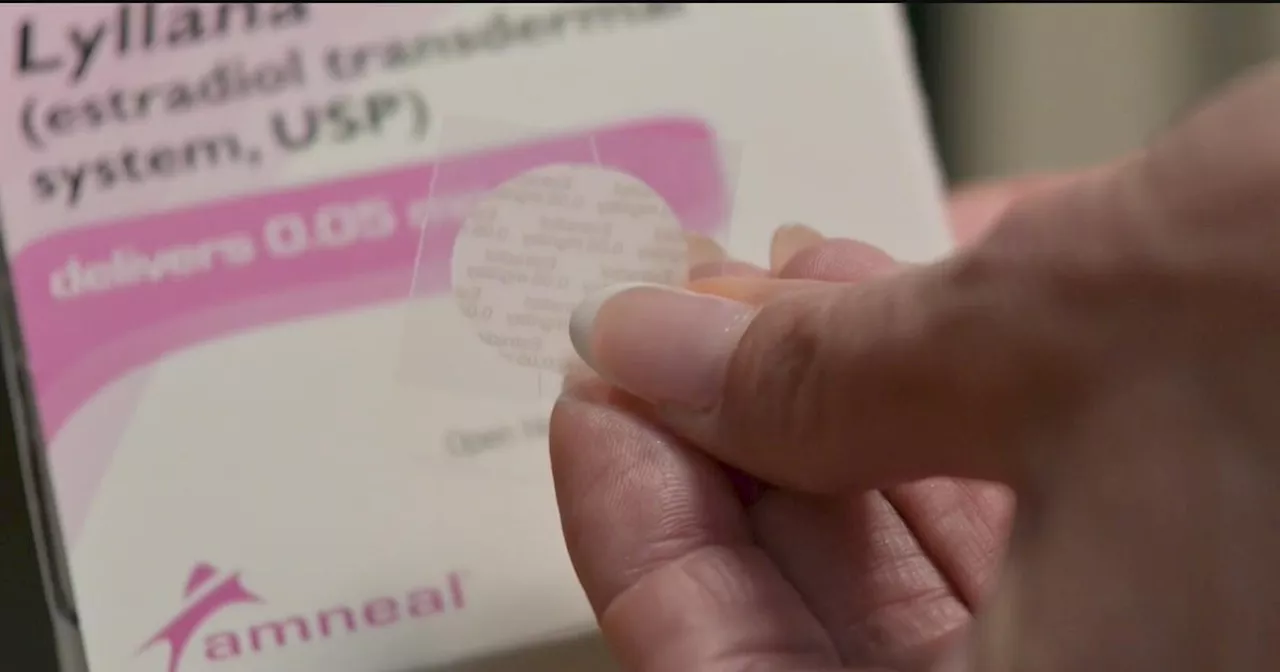
A significant shortage of estrogen patches is impacting women across the United States seeking hormone replacement therapy (HRT) to alleviate symptoms associated with menopause and perimenopause. This shortage has been driven by a notable increase in demand, which has surged by 72% since 2021, according to a study by Epic Research. The escalating demand is largely attributed to heightened awareness of menopausal health and recent changes from the U.S. Food and Drug Administration (FDA) regarding hormone therapies.
Pharmacies nationwide are struggling to keep up with the demand for estradiol patches, leaving many women to face the challenges of managing debilitating symptoms. The issue is compounded by supply chain disruptions and the lack of insurance coverage for brand-name alternatives, making it difficult for patients to find suitable treatments.
Martie Jo Pennisi, a resident of Glendale, California, began experiencing severe menopause symptoms in October 2020. “I was kind of crawling out of my skin, and really the symptoms came on like gangbusters,” she explained, detailing struggles with depression, anxiety, and extreme hot flashes. After consulting a friend, she decided to pursue HRT and started using an estradiol patch along with a progesterone pill in the spring of last year.
While her symptoms improved significantly, Pennisi faced a setback when she attempted to refill her prescription last month. Her pharmacy informed her that the estradiol patch was unavailable. “I contacted multiple pharmacies across the county, but none had the estradiol patch in stock,” she said.
Dr. Jessica Shepherd, a menopause expert, noted that the current shortage reflects a dual narrative of progress and ongoing challenges. “The good news is that more women are asking for estradiol in the form of a patch,” she stated. “The bad news is that we see a supply chain issue. This is not just one particular pharmacy; this really is across the board.”
The FDA’s recent decision to remove the boxed warning from certain hormone therapies has been cited as a factor in the increased demand. As awareness of menopause and its management options grows, more women are seeking treatments that were historically shrouded in stigma. Pennisi observed that women in her family endured menopause quietly, without open discussions about their experiences. “Nobody in my family, not my mother, my grandmother, my sisters, nobody,” she lamented.
In light of the shortage, Dr. Shepherd advises patients to discuss alternative forms of estradiol with their healthcare providers. Options such as creams, gels, pills, or pellets may be viable substitutes. “There is no difference in how it works,” she explained. “Some people may notice differences in how their body responds, but you’ll never know until you try it.”
Ultimately, Pennisi managed to find a weekly estradiol patch instead of her usual twice-weekly version. Although she is relieved to continue her treatment, she expressed frustration with the situation. “If the world experienced men losing all their testosterone at once, there would be a whole different story,” she remarked, highlighting the ongoing fight for better awareness and treatment options for women’s health issues.
As many women navigate the shortage, some have opted to switch from generic to brand-name hormone treatments. Unfortunately, these alternatives often come with high costs, sometimes amounting to hundreds of dollars per month, which may not be covered by insurance. This adds yet another layer of difficulty for patients seeking effective relief from their symptoms.
As the healthcare community continues to address these shortages and advocate for improved access to treatment, the journey for many women remains filled with challenges.